Timely prediction is key to saving both lives and money in the health care system. I recently talked to Sam Yang, managing director and cofounder of Xandar Kardian, about their motion sensor called XK300 that can tip off clinicians to oncoming emergencies in patients suffering from COVID-19, heart failure, COPD, pneumonia, asthma, and more.
The XK300 (Figure 1) emits very fast, high-bandwidth signals over a wide area in a technology called ultra wide band (UWB) radar. The XK300 is pretty tolerant of location; it can be on a wall or even a ceiling (which would make it harder to remove) and can scan an entire human body (Figure 2). Thus, it can check the breathing and even the heart beat of a sleeping patient. The device has FDA clearance and Xandar Kardian markets it both to hospitals and to clinicians monitoring patients in their homes.

Take the example of rapid breathing, a common indicator of risk in COVID-19 patients as well as those with asthma, pneumonia, and heart disease. A healthy breathing rate of a person at rest is around 10 to 12 breaths per minute. If those goes up a bit—say, to 15 breaths per minute—there’s an early sign of lung or heart problems that could get worse fast.
The XK300 can detect a change from 12 to 15 breaths per second. In contrast, a pulse oximeter reports a problem only when breaths get up to about 25 per minute. The person is quite close to an emergency by that time.
Yang mentioned the new Merck COVID-19 pill as a treatment where timing is critical. Patients benefit greatly from the early detection of breathing problems provided by the XK300, if they can get the Merck pill.
The famous 30-day rule (where Medicare penalizes hospitals whose patients are readmitted 30 days after discharge) provides a home use case for the XK300. The information the device collects, as appropriate, can include lack of motion, number of exits from the bed, and time spent in the bathroom, which gives useful information about patient habits and can anticipate a urinary or kidney problem. Xandar Kardian is working on getting FDA approval for detecting sleep apnea.
Many clinicians and patients are finding the XK300 preferable to wearable devices, Yang claims. Many patients remove the wearable as soon as they feel well, or just forget to use it. These devices are also limited to measuring what they can sense at the particular part of the body where they’re worn.
Wearables, of course, have the advantage of going wherever the individual goes, and therefore are useful for tasks such as measuring how many steps you’ve taken each day. Accuracy varies: some devices are accurate within a few hundred steps. Fitness trackers actually do worse than smart phones, and devices are not so good at measuring sleep.
The highly accurate XK300 can be used for continuous monitoring, but also generates useful information in a short period of time (Figure 3). The device is normally placed near a bed or chair.
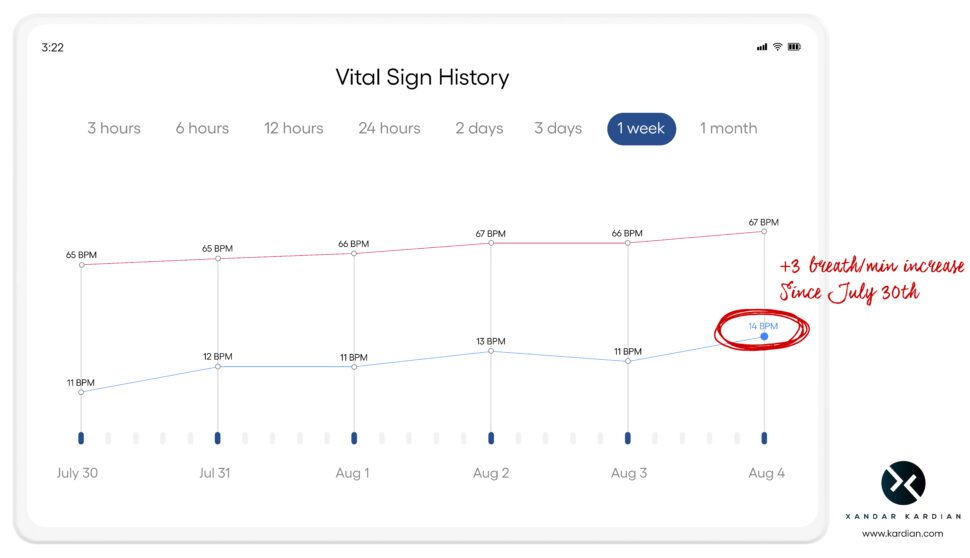
A lot of intelligence is built into the XK300. For instance, if the patient is moving around in bed, the device doesn’t count the breathing in determining the average breath rate at rest. I asked Yang whether the XK300 could distinguish between a human and a cat or dog. He said they couldn’t do that, but had a solution for people with pets: a pendant hung around the pet’s neck that warns the XK300 when it’s picking up signals from the pet.













