ACOs saved Medicare $755M from 2013 to 2017, new analysis finds
FierceHealthIT
DECEMBER 2, 2019
Accountable care organizations lowered Medicare spending by $755 million from 2013 to 2017, a new analysis found.
This site uses cookies to improve your experience. By viewing our content, you are accepting the use of cookies. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country we will assume you are from the United States. View our privacy policy and terms of use.

FierceHealthIT
DECEMBER 2, 2019
Accountable care organizations lowered Medicare spending by $755 million from 2013 to 2017, a new analysis found.

Electronic Health Reporter
JANUARY 20, 2020
In the fall of 2013, when cancellation letters—notices of cancelled plans—went out to approximately four […]. The article The Doctor Won’t See You Now: The Unintended and Perhaps Inevitable Consequences of Medicare-for-All appeared first on electronichealthreporter.com. But the promise was impossible to keep.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.

FierceHealthIT
MARCH 14, 2019
The Centers for Medicare & Medicaid Services released its updated dashboards with new prescription drug pricing and spending data on Thursday. Among its findings, Medicare spending on prescription drugs grew by more than 10% between 2013 and 2017, while Medicaid spending grew by nearly 15%.

FierceHealthIT
OCTOBER 2, 2018
Of the nearly $7 billion Medicare paid to inpatient rehab hospitals in 2013, $5.7 billion was deemed improper. The watchdog agency recommended that CMS revamp its payment structure for rehab hospitals.

Digital Health Global
OCTOBER 17, 2023
1 Centers for Medicare & Medicaid Services (CMS). Public Use Files (Medicare Claims) – Medicare Physician & Other Practitioners – by Geography and Service 2013-2020. 2 Centers for Medicare & Medicaid Services (CMS). Standard Analytical Files (Medicare Claims) – LDS 2021.

American Well
JUNE 25, 2017
the Helping Expand Access to Rural Telehealth (HEART) Act targets the Center for Medicare & Medicaid Services’ (CMS) strict limitations on RPM reimbursements in rural areas. Of the 107,000 telemedicine visits for Medicare beneficiaries recorded in 2013, approximately 40,000 of them served rural areas. Sean Duffy (R-Wis.)

American Well
JUNE 25, 2017
the Helping Expand Access to Rural Telehealth (HEART) Act targets the Center for Medicare & Medicaid Services’ (CMS) strict limitations on RPM reimbursements in rural areas. Of the 107,000 telemedicine visits for Medicare beneficiaries recorded in 2013, approximately 40,000 of them served rural areas. Sean Duffy (R-Wis.)
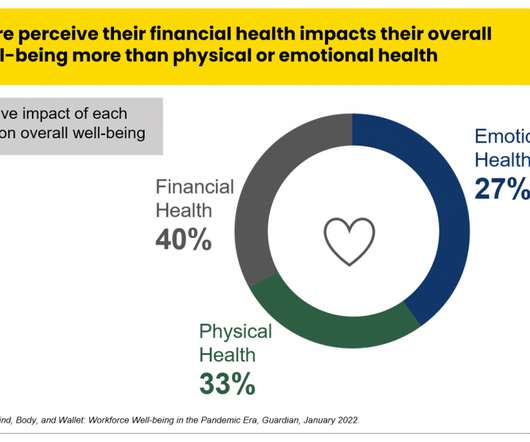
Health Populi
JUNE 23, 2022
points which was the biggest two-week decline in the past year — and the lowest level since CivicScience launched this study in 2013. billion savings that Medicare Part D could accrue if the program bought generic drugs at the prices offered through the Mark Cuban Cost Plus Drug Company. Yes, that Mark Cuban).

Digital Health Wire
NOVEMBER 20, 2022
DispatchHealth launched in 2013 to bring urgent care into patient homes, but has since expanded its offerings to cover a wide range of high-acuity needs. It looks like 2022 isn’t finished with the megarounds quite yet, with DispatchHealth hauling in $330M in a mix of debt and equity funding to build out its suite of in-home services.
Lloyd Price
NOVEMBER 5, 2018
With two months left in 2018, healthcare startups have already raised more in VC funding this year than they did in all of 2012 and 2013 combined, according to an analysis conducted for Forbes by Pitchbook. In 2012 and 2013 combined, the sector raised $22.3 billion in 12 months. So far this year that $26.3 So far this year that $26.3

Aging in Place Technology Watch
OCTOBER 29, 2020
In fact, 2013-2017 saw the rise, rise, and then fall of Home Hero – which raised $18 million, closing in 2017 and Hometeam’s $40 million in 2016. . In 2019, Medicare Advantage began covering some non-skilled home care. Why the froth? Homecare a sizable and growing market. In 2019, the private duty home care market was sized at 23.5

Healthcare IT Today
APRIL 28, 2023
billion through Arcadia’s Medicare Shared Savings Program (MSSP) service. Since formation in 2013 and as of December 31, 2022, VCP has deployed over $9.7 The past year included several important milestones for Arcadia, including: Inclusion on Inc. billion and grown to over $6.6 billion of assets under management.

Healthcare IT Today
FEBRUARY 27, 2024
HealthBeacon was founded in 2013 in Dublin, Ireland. The product is patent protected, FDA cleared, and FSA, HSA, Medicare, and Medicaid eligible. Postal Service’s approved mail-back program. HealthBeacon also provides a digital risk management platform for prescribing restricted medication to oncology patients.

ACA Times
DECEMBER 1, 2015
in 2014, and overall health spending grew by 5.3%, according to the Centers for Medicare & Medicaid Services (CMS) , a slower rates of growth than most years prior to passage of the Affordable Care Act. growth in 2013, reflecting the increased number of individuals with health coverage, according to CMS. growth in 2013.

BHM Healthcare Solutions
MAY 11, 2023
Another example of a payvider is Alignment Healthcare, a Medicare Advantage plan that also offers primary care services. Alignment Healthcare was founded in 2013, and it currently operates in several states across the US.

ACA Times
JULY 28, 2015
Analyzing data compiled by Medicare, the newspaper found that the number of nurse practitioners receiving payments from the program rose by 15% in 2013 compared to the previous year, and by 11% for physician assistants. By contrast, the number of general practice physicians paid by Medicare declined by 5% from the prior year.

Electronic Health Reporter
JULY 23, 2018
The successor to the 2013 BPCI program, BPCI Advanced is CMS’ most significant episodic payment reform proposal to date, indicating the government’s […]. The Bundled Payments for Care Improvement (BPCI) Advanced initiative is a new advanced alternative payment model (APM) that will go live October 1, 2018.

ACA Times
APRIL 7, 2015
Physicians have been accepting a smaller percentage of new Medicaid patients than patients on Medicare or with private insurance, according to a study by the National Center for Health Statistics (NCHS), part of the Centers for Disease Control. The NCHS looked at the acceptance of new patients by doctors in cities and smaller communities.

Henry Kotula
OCTOBER 6, 2018
Between 2013 and 2017, 64 rural hospitals closed due to financial distress and changing healthcare dynamics, more than twice the number in the previous five years, a new Government Accountability Office analysis shows. . GAO also looked at closures by Medicare rural hospital payment designation. Dive Brief: Hospitals across the U.S.

BHM Healthcare Solutions
MARCH 19, 2019
Editor’s Note: Increasing costs for prescriptions is creating a long-term financial impact on Medicare Part D and its beneficiaries. For its report, the CDC analyzed National Health Interview Survey results from 2013-17. Can your claims review resources maximize the turn around time needed for complex claims?

Healthcare IT News - Telehealth
OCTOBER 19, 2020
In the suit, the EHR giant argues that it has used the CarePort trademark since 2013 and that in 2018 the telemedicine company changed its name from ER at Home to CarePortMD. Earlier this summer, CarePort launched a tool to help hospitals comply with the Centers for Medicare and Medicaid Services' interoperability final rules.

Digital Health Global
MARCH 31, 2023
As a result, Wellth’s health plan and provider clients have measured drastic cost savings, and Medicare Advantage plans have achieved higher Star ratings. The core of its value-add is Beacon, the AI engine SignalFire has been refining since the firm’s launch in 2013.

BHM Healthcare Solutions
JANUARY 8, 2019
Editor’s Note: Increasing costs for prescriptions is creating a long-term financial impact on Medicare Part D and its beneficiaries. Between 2013 and 2015, prices rose by nearly 10 percent, six times the rate of general inflation. Can your claims review resources maximize the turn around time needed for complex claims?

American Well
MAY 25, 2016
28% Annual Increase in Telemedicine Visits Provided to Medicare Beneficiaries. Harvard Medical School researchers found that the number of telemedicine visits provided to Medicare beneficiaries increased by 28 percent per year from 2004 to 2013 with 107,000 visits provided in 2013. Medical Xpress. visits per patient.

ACA Times
MARCH 15, 2017
The Center for Consumer Information & Insurance Oversight (CCIIO), under the Centers for Medicare & Medicaid Services (CMS), released a notice at the close of February, announcing that insurance companies may extend coverage of certain non-grandfathered individual and group plans that are currently not ACA compliant for another year.

Aging in Place Technology Watch
SEPTEMBER 6, 2022
increase in revenue from 2013 to 2020. And that the costs (estimated at $754 million in 2015) were mostly paid by Medicare and Medicaid (the latter likely in nursing homes.) Consider their newly published document explaining the industries to those who may still not see what’s happening. Census Bureau projects that in 2050, the U.S.

CMS.gov
MARCH 1, 2019
Administrator, Centers for Medicare & Medicaid Services. Medicare Parts A & B. My primary mission as the Administrator of the Centers for Medicare and Medicaid Services (CMS) is to deliver on President Trump’s commitment to strengthen and modernize Medicare for the millions of Americans who depend on us every day. .

ACA Times
AUGUST 20, 2015
The studies were released by the Urban Institute in partnership with the Robert Wood Johnson Foundation; the National Center for Health Statistics of the Centers for Disease Control and Prevention; the Centers for Medicare & Medicaid Services; and Gallup, Inc. in 2013 to 9.1% in 2013 to 9.1% to 9.0%; Oregon, 19.4%

Healthcare IT News - Telehealth
JULY 18, 2022
"Since 2013, we had provided e-consults as one of the original AAMC Project CORE institutions," she added. "In 2019, UVA Health created a multi-stakeholder strategic plan for telemedicine.

Health Populi
JUNE 7, 2018
Some key findings from this study were that: The fastest-growing spending conditions between 2013 and 2014 were infectious disease, mental illness, and diabetes. The second chart indicates healthcare spending by category in billions of dollars and annual rate of growth.

ACA Times
APRIL 20, 2016
Over the course of ten years—from 2004 to 2014—Medicare has increased its funding of prescription drug costs from 2% to 29%. 86% of Americans feel drug companies should release information on setting drug prices, while 83% suggest Medicare should negotiate to lower those prices. Specialty drug costs saw an increase to 30.9%

Enzyme Health
JULY 31, 2019
Medicare currently covers many telehealth services depending on coverage level and geography, but still faces some restrictions, with Medicare Advantage plan beneficiaries (about 14 million patients) receiving the broadest access ( ATA Telehealth Basics ). million in 2013 to a projected 7 million in 2018 ( Statista ).

ACA Times
MAY 1, 2019
Department of Health and Human Services’ Center for Medicare and Medicaid Services (CMS) has extended the period of non-enforcement for certain non-compliant health policies under the Affordable Care Act through the end of 2020. 2 minute read: The U.S.

Insulin Nation
APRIL 24, 2015
Reegan Karice Oxendine was a toddler when she died in September 2013 from undiagnosed Type 1 diabetes. North Carolina is one of 18 states not participating in the Medicare Expansion Plan. She became noticeably sick beginning at 14 months of age, and her parents took her to the doctor numerous times.

Medicine and Technology
FEBRUARY 13, 2013
Despite what you hear, Medicare reimbursement is not the Holy Grail for telemedicine. It’s important, but… Medicare fee-for-service covers about 36 million Americans, 12 percent of the total U.S. But devices are TOOLS that allow services to be provided at a distance. population.

LinkousThink
DECEMBER 13, 2012
For example, the cliff would cut Medicare hospital related payments by 2 percent, but suggested alternatives could cut even more. In the health care world, one part of the “cliff” is an automatic 27% cut January 1 in Medicare fees for physicians and other practitioners. But here’s the problem – we’re stuck in the trunk!

Medicine and Technology
FEBRUARY 18, 2013
How about listening to a webinar on our heatlhcare ecosystem?

Insulin Nation
AUGUST 20, 2015
In April 2013, the FDA published a report entitled “Strengthening Our National System for Medical Device Postmarket Surveillance.” He’s helped lead a lobbying effort to persuade Congress to require Medicare to pay for the services of certified diabetes educators and to cover the expense of continuous glucose monitors.

Health Blawg
APRIL 30, 2018
The company supports provider organizations participating in the BPCI program , having gone live in Fall 2013. Aprima belongs to CommonWell, has done some FHIR development, and Michael would like to see Congress condition Medicare reimbursement on real interoperability.

Health Blawg
APRIL 30, 2018
The company supports provider organizations participating in the BPCI program , having gone live in Fall 2013. Aprima belongs to CommonWell, has done some FHIR development, and Michael would like to see Congress condition Medicare reimbursement on real interoperability.

Health Blawg
APRIL 30, 2018
The company supports provider organizations participating in the BPCI program , having gone live in Fall 2013. Aprima belongs to CommonWell, has done some FHIR development, and Michael would like to see Congress condition Medicare reimbursement on real interoperability.

Health Blawg
APRIL 30, 2018
The company supports provider organizations participating in the BPCI program , having gone live in Fall 2013. Aprima belongs to CommonWell, has done some FHIR development, and Michael would like to see Congress condition Medicare reimbursement on real interoperability.

Health Blawg
APRIL 30, 2018
The company supports provider organizations participating in the BPCI program , having gone live in Fall 2013. Aprima belongs to CommonWell, has done some FHIR development, and Michael would like to see Congress condition Medicare reimbursement on real interoperability.

American Well
SEPTEMBER 27, 2015
Medicare Telehealth-Based Chronic Care Management. Telehealth and the Medicare Access and CHIP Reauthorization Act. Travel payment savings for Year 1 of the study–which examined all telemedicine visits at the VA Hospital in White River Junction, Vermont, from 2005 to 2013–were $18,555. Telehealth and New Payment Approaches.
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content